Joint pain frequently disrupts daily routines and limits physical mobility for countless individuals. Many people rely on anti-inflammatory medication or invasive surgery to manage these persistent symptoms. Regenerative medicine presents a promising alternative by focusing on biological restoration rather than simple symptom suppression. This evolving field aims to repair damaged tissues through the body’s own potent healing mechanisms.
What Is Regenerative Medicine?
Regenerative medicine centers on the scientific process of replacing or engineering human cells. Physicians utilize this specialized approach to restore normal function in damaged tissues or organs. The strategy shifts the clinical focus from temporary management to actual physiological repair.
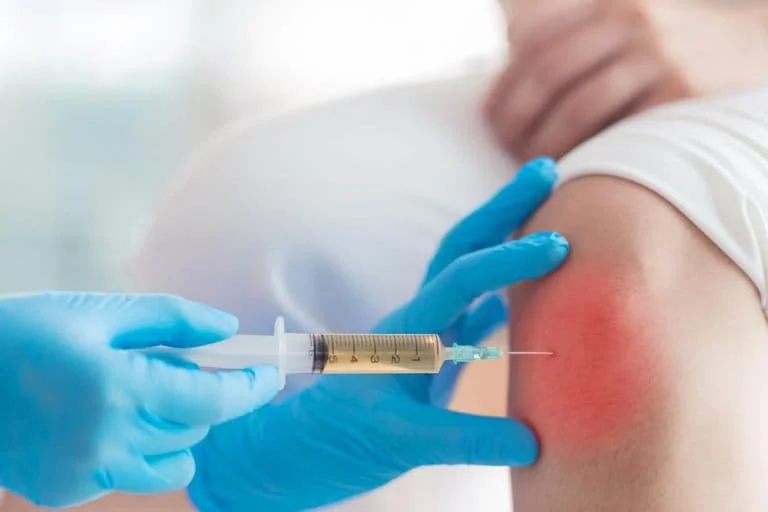
The human body holds a remarkable capacity for self-healing after a traumatic injury occurs. Scientists develop targeted therapies that harness and amplify this natural biological potential. These treatments often involve the injection of biological substances directly into the affected joint space.
This medical discipline continues to grow as researchers understand more about the body’s healing pathways. Clinical studies investigate how these therapies can delay or prevent the need for joint replacement surgery. Patients increasingly seek these options to maintain an active lifestyle without extensive downtime.
Which Treatments Are Innovative?
Medical professionals currently use several advanced therapies to address joint deterioration and chronic pain. They derive these potent biological materials from the patient or ethical donor sources. The selection of a specific therapy depends largely on the injury type and severity.
- Platelet-Rich Plasma (PRP): Doctors spin a patient’s blood sample to concentrate platelets that release proteins to aid tissue repair.
- Bone Marrow Concentrate: Specialists harvest stem cells from the patient’s pelvis to support the regeneration of cartilage and bone.
- Prolotherapy: This method uses a dextrose solution to trigger a localized healing response in weakened ligaments.
Researchers are actively studying these specific applications to confirm their effectiveness in providing long-term relief from joint pain. As part of this ongoing research, they consistently refine the harvesting and injection techniques to maximize positive patient outcomes and improve the healing process. These procedures are typically straightforward and convenient, as you can usually undergo them in a standard outpatient clinic environment without the need for a hospital stay.
Who Is a Candidate?
Determining candidacy requires a thorough medical assessment by a qualified orthopedic physician. Doctors look for patients who have exhausted other non-surgical options without success. The ideal candidate maintains good overall health despite their specific joint issues.
- Mild to moderate osteoarthritis
- Chronic tendon injuries
- Ligament sprains or tears
- Meniscal tears
Certain lifestyle habits influence the body’s ability to respond to these biological treatments. Smoking often restricts blood flow and impedes the necessary healing response within the tissue. Your doctor will review your history to see if regenerative medicine fits your needs.
Consult a Specialist
You need a professional evaluation to determine the best course of action for your joint pain. Schedule a consultation with a specialist to discuss your specific condition and recovery goals. The doctor will perform a physical exam and review your diagnostic imaging results. This visit clarifies whether regenerative medicine offers a viable path for your recovery. Taking this step empowers you to make informed decisions about your future joint health.